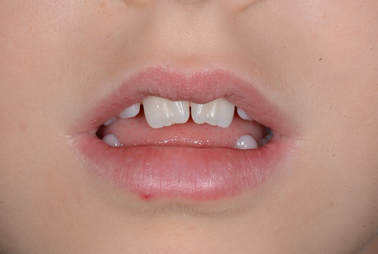
 Patient "Miss A", with evidence of mouthbreathing and a forward tongue. © 2018 Dr Chris Baker Patient "Miss A", with evidence of mouthbreathing and a forward tongue. © 2018 Dr Chris Baker Funny how we call detailing the tooth alignment and the bite, “finishing”. Funny because it all starts from diagnosis. Actually it starts at the initial examination. What we do at the beginning makes our finishing time longer or shorter.
Here are three examples of finishing challenges that can become overwhelming, and how you can know of the facts, and handle the challenges better, from the start: Facts and challenges like: Patient Miss A may need lengthy and difficult anterior bite closure - how do you know?.
- ENT referral and treatments - Tongue exercises that you prescribe - Sublingual frenectomy - Habit treatment - Bite turbos, posterior biteplate, or other posterior intrusion therapies - UAW or other molar positioning and incisor extrusion where appropriate - TAD anchorage with posterior intrusion - Lower full coverage splint following ortho treatment And look at the concern typed onto the treatment plan for this patient, just above the signature line for the parent/patient: Concern – Airway issues, habits and adverse tongue positions all contribute to adverse growth and continued adverse forces on teeth, with or without orthodontic treatment. Adam’s growth is vertical, which is made worse by mouth-breathing and low tongue position. This may predispose him to an openbite. All treatment will be directed to improving these adversities, but longterm stability is lessened and risk of relapse is greater, depending on the success of the airway treatment, tongue position improvement and habit cessation. OR Vertical growth patterns are difficult to correct, and when corrected, often relapse, with a return of the open bite (space between upper and lower incisors, when the patient is biting on the posterior teeth.) Even in the best-case scenario, openbites may relapse. Beginning treatment as soon as is feasible may help in longer-term stability. Compliance with elastic wear, if indicated, is important. All treatment is directed to improving the openbite pattern with as much stability as possible. Annie’s tongue position is low and forward, and probably is contributing to the spacing of her teeth. Tongue training may be helpful, including CM circle and ball on retainers, and wear of her retainers as directed, will be critical, because the teeth often exhibit connective tissue memory/relapse without excellent retainer wear, due to the tendency of the tongue to remain forward and low throughout life. Patient Mr. B may have later excessive mandibular growth, “outgrowing” your orthodontic treatment that attained a beautiful Class I, and the patient ends up Class III with open bite tendency. How do you know?
A patient and his mother presented for a recall orthodontic evaluation, and the mom said her dentist had asked her why we took the braces off, when he had 0 overbite and 0 overjet. A review of his final photographs at orthodontic completion showed a Class I occlusion with 3 mm overbite and 3 mm overjet. Indeed that was not the case any longer. His treatment plan had listed the concern of possible excessive mandibular growth. He had a chin sling for nighttime wear prescribed for wear with his retainers, which had not been worn. Don’t we dislike these concerns expressing themselves in reality? But - we don’t make the growth, and we are pleased to stress the concern at the diagnostic and retainer delivery stage. The patient compliance may not work to advantage. We hate that, of course. Treatment during or throughout the original active phase, not just during what we call finishing may include: - Class III Correctors - Motion or D2 appliances - Chin Sling or Facemask wear - Posterior intrusion therapies Communication of growth progress to the parent is critical, throughout treatment. Keep them in the reality loop! Patient Miss C may have difficulty attaining and maintaining adequate canine and/or posterior overbite. How do you know?
- Tongue exercises - Blue Grass or other beads in palate - Castillo-Morales circle in palate - Crib on appliances - Expansion therapy We could similarly lay out the signs of future TMJD, of lack of eruption of an ectopic tooth, adding 2-3 years to a treatment time, of the complete dependence on the patient’s compliance if the occlusion is to be corrected, and on and on… So, before you even consider putting appliances into a patient’s mouth, consider the findings - all of them. Do excellent diagnostics. Get all the information - about medical, airway and breathing, dental, skeletal, growth and finally dental findings. THEN put it together in a comprehensive treatment plan that you can share with the parent /patient, giving them the information they need to make good informed decisions about the treatment. Then, pay the closest attention to your bracket placement. Bracket placement, though impossible to do perfectly, can make huge differences in finishing needs. Keep everyone — parents, patient, your chart — in the loop. Be honest and open with the progress, OR LACK THEREOF. This will help you throughout the treatment. Your finishing will be more predictable, and could be a lot less surprising, a lot less difficult, and a lot less stressful for all.
0 Comments
Leave a Reply. |
Dr Chris BakerAmerica's most-trusted teacher of orthodontic continuing education, Dr. Chris Baker has practiced and taught for more than 30 years, and is a current or former faculty member of three U.S. dental schools. She is a pediatric dentist, author, blogger, dental practice consultant, and mentor. Dr. Chris is also Past President and Senior Instructor of the American Orthodontic Society. She is based in Texas, USA, but lectures around the world. Categories
All
Archives
April 2024
Text and images
© 2023 Dr Chris Baker |


 RSS Feed
RSS Feed