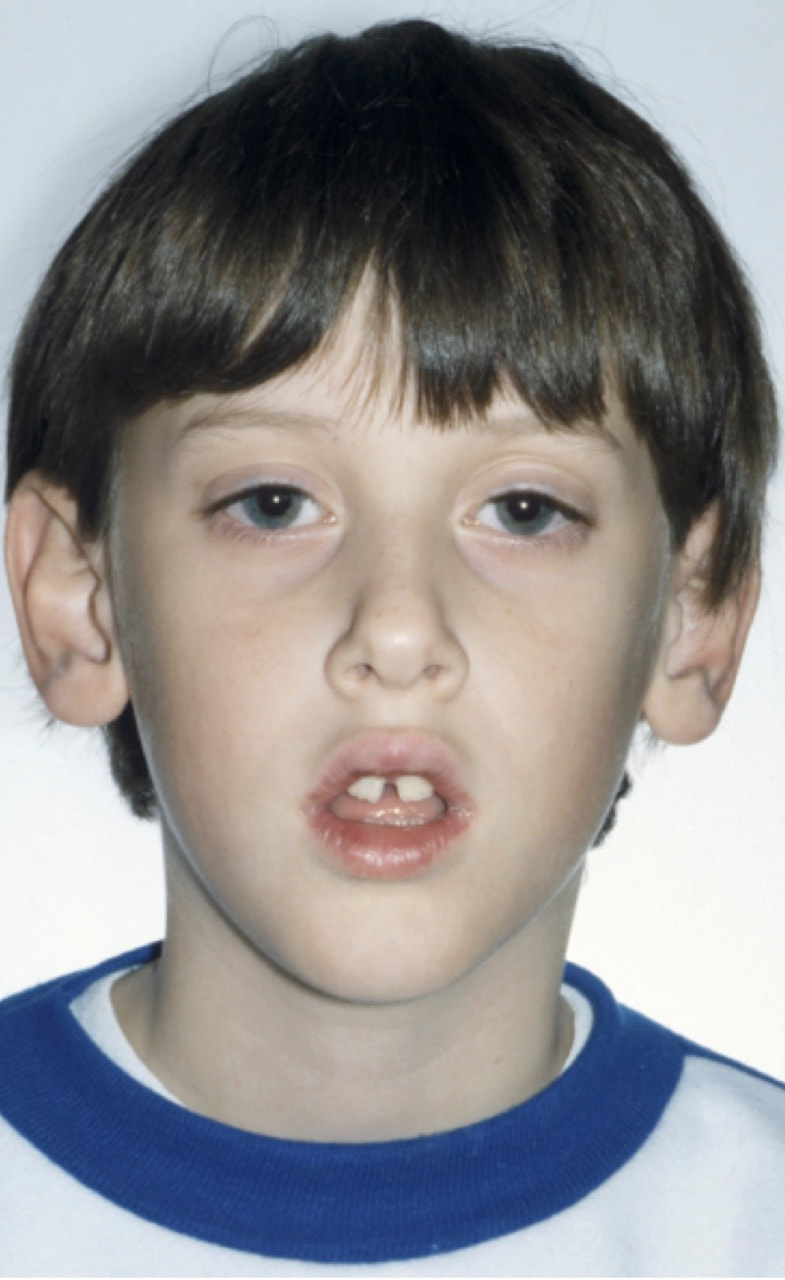
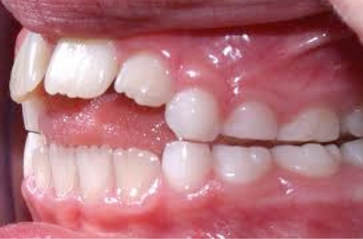
Instead of Edwin having Class III brachyfacial growth which he “inherited” from Dad who looks the “same,” the child has a severe forward tongue position, with deep bite, forward mandibular positioning and Class III growth. It is indeed the “same” as Dad - both Edwin and his dad spent early formative years with huge tonsils and inability to breathe nasally. Breathing is primary. We do what we must to breathe. Unknowingly posturing his mandible forward, bringing the tongue with it, due to the hyoid muscle attachments, allows Edwin, and allowed his father, to breathe through his mouth, bypassing his nose, and get the oxygen needed to survive. So - Dad and Edwin grew similarly - Class III. The genetic etiology for this father and son pair has to do with tonsillar enlargement - and in Edwin’s case - is CHANGEABLE because he is still growing. Following removal of the tonsils and adenoids (adenoid tissue was enlarged as well), and expansion of his narrow palate, Edwin now breathes nasally. His Class III growth is diminishing (still habitual forward tongue.…). As an early evangelist with this subject, having learned from Dr. Walter Doyle, I discovered that there was a huge volume of airway literature produced in the 1970’s, much of it led by Sten Linder-Aronson and Donald Woodside, Dudley Weider, Kenneth Nowak and colleagues, Donald Timms, and even Henri Petit. They knew and published about what we think we are so smart to be “figuring out” now. Having been teaching and practicing this knowledge all these 25+ years, I am - yes - THRILLED - to see our “modern” thinking catching up to this body of knowledge. 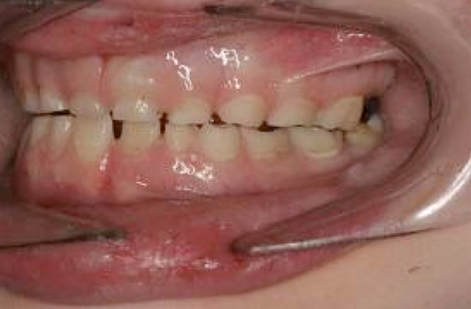 Upper airway congestion is etiologic in childhood bruxism (tooth grinding). Image and text © 2001 Dr Chris Baker Upper airway congestion is etiologic in childhood bruxism (tooth grinding). Image and text © 2001 Dr Chris Baker Five things your patient may exhibit which could indicate airway issues: While we could spend hours on this topic - and I do in teaching - for now let’s just look at five things your patients might exhibit to let you know they have an airway problem or may have an airway problem. Because - if your patient begins breathing nasally, their growth and development is changed - starting immediately. So the five things? 1. Enuresis - Bedwetting; 2. ADHD, ADD, behavioral problems, manic-depressive disorder of childhood, aggressive behavior; 3. Lowered IQ and Learning disabilities; 4. Restless sleep and daytime fatigue; 5. Bruxism - tooth grinding. These all reduce a child’s quality of life - experience of life - to a life with difficulties, struggles, and are very often changeable, thus unncecessary. And you can be the one to guide the life-transformation. "Normal healthy cells turn into malignant cells simply in the presence of lowered O2." ~ Otto Warburg Three things you can do to improve the child’s chance of nasal breathing and his/her life You - the child’s orthodontist, dentist, pediatric dentist, can help - a LOT!! You can:
Nasal and sinus mucosa release nitric oxide, a potent bronchodilator and vasodilator, hypotensive and it is bacteriostatic and virostatic. There is more - so much more we can discuss about this topic. Can you imagine, the lives you can change? Can you imagine, how grateful the parents will be? Can you imagine reducing the risk of adult sleep apnea in your now child patients? Can you imagine, how wonderful for you? Learn about the airway in children. Contact me and I will be glad to help.
1 Comment
Arafa mohamed Khatab
12/7/2017 08:44:12 am
Nice
Reply
Leave a Reply. |
Dr Chris BakerAmerica's most-trusted teacher of orthodontic continuing education, Dr. Chris Baker has practiced and taught for more than 30 years, and is a current or former faculty member of three U.S. dental schools. She is a pediatric dentist, author, blogger, dental practice consultant, and mentor. Dr. Chris is also Past President and Senior Instructor of the American Orthodontic Society. She is based in Texas, USA, but lectures around the world. Categories
All
Archives
July 2024
Text and images
© 2024 Dr Chris Baker |


 RSS Feed
RSS Feed